First Aid and CPR for Infants and Toddlers - A Guide for Parents and Caregivers


First Aid and CPR for Infants and Toddlers - A Guide for Parents and Caregivers
 By Inventive Minds Kidz Academy
By Inventive Minds Kidz Academy
 Added Wed, Mar 06 2024
Added Wed, Mar 06 2024
 By Inventive Minds Kidz Academy
By Inventive Minds Kidz Academy
Added Wed, Mar 06 2024
Hey, Thanks For Subscribing!
Please check for a confirmation message and ensure you add us to a safe email list.
If you don't see a message in the next five minutes, check your spam or junk folders and mark our emails safe for next time.
See you soon!
Duplicate Email Found!
Well this is embarrassing... It looks like is already registered.
We have just sent an email to that address with a link to manage the subscription with us. If you don't see a message in the next five minutes, check the spam or junk folders, it's definitely there.
See you soon!

As a parent or caregiver, our primary responsibility is to make sure our little ones are safe. Accidents may happen at any time, especially to children who are more curious and playful. In this guide, we will discuss essential first aid techniques specifically tailored for infants and toddlers, and young age groups. Fast and informed action can make all the difference when it comes to emergency situations.
In this article, first we will discuss the principles of CPR (Basic Life Support), Then we will discuss other common emergencies in which a child may need immediate help.
Cardiopulmonary Resuscitation:
Infants and toddlers are prone to accidents due to their curiosity and not yet developed motor skills. Common emergencies include falls, choking, burns, allergic reactions, and seizures. As a caregiver, you should be vigilant and look for signs of an emergency.
1. Assess the situation:
The first thing to do when assessing the situation is to make sure that it is safe for you to help the child in need. Assess the environment for hazards such as traffic, sharp objects, or electrical dangers. If all is clear, attend to the child. Check for responsiveness. Gently tap the child’s face and shout to get the child’s attention, use their name if known. Look quickly to see if the child has any injuries, bleeding, or medical problems, do not spend more than 10 seconds at this stage.
If there is no response, check for breathing. Place your ear near the child’s mouth and nose. Your face should be towards the child’s chest. Is there breath on your cheek? Is the child’s chest moving? CPR is indicated only for unresponsive and non-breathing children.
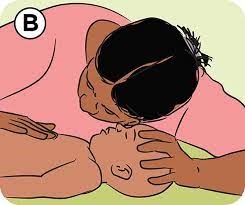
2. Call for help:
As mentioned earlier, if the unconscious child is breathing normally, there is no need for CPR (Cardiopulmonary Resuscitation). Immediately call 911 and ask for help.
If the child is not breathing or is gasping for fresh air, you should start CPR right away.
If you’re not alone, ask the other person to call 911 and then look for an AED as you start the CPR, but if you’re alone, don’t postpone the CPR for calling 911. Start the CPR immediately, and after 2 minutes of effective CPR, call 911 and look for an AED.
3. Start the CPR:
To start the CPR, put the child on a firm, flat surface.
For children under 1 year old, start by placing both of your thumbs in the center of the baby’s chest, just below the nipple line. Use your other fingers to encircle the baby’s chest and provide support. Push down hard and fast. You can also use your index and middle fingers and do the chest compression with one hand, as shown below. The depth of a push should be about one and a half inches. The rate should be 100–120 pushes per minute. Use rescue breaths on a regular basis. If you are alone, the ratio of chest compressions to rescue breaths should be 30:2. If there is another person helping you, the recommended ratio is 15:2.
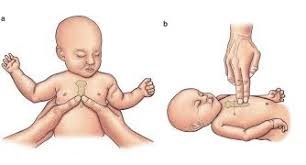
For performing a rescue breath, tilt the child’s head slightly backwards and lift the child’s chin slightly upwards to make sure the airway is open. Then take a breath, put your mouth around the baby’s mouth and nose to make a seal, and blow gently and steadily for up to one second. The chest should rise. Remove your mouth and watch the chest fall. That’s one rescue breath. You should take two rescue breaths in each cycle.

For Children above 1 year age Place the heel of one hand in the center of the child’s chest, and use your other hand on top, fingers interlaced, and off the child’s chest. Position your shoulders directly over your hands and lock your elbows. Push down hard and fast for about 2 inches at a rate of 100 to 120 compressions per minute. Allow the chest to return to its normal position after each compression. Use rescue breaths with the ratio provided earlier (30:2 if you are alone and 15:2 if there are 2 rescuers).
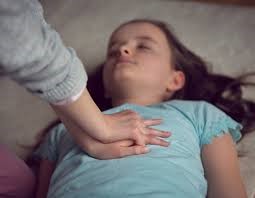
Check for breath every 2 minutes (every five 30:2 cycles). As mentioned before, if you are alone, you can call 911 and look for AED after about 2 minutes (five cycles).
4: Use the AED as soon as it is available:
For children age 9 and under, use a pediatric automated external defibrillator (AED), if available. If a pediatric AED is not available, or for children age 1 and older, use a standard AED.
First, turn on the AED. Then, wipe the chest dry and attach the pads. The AED will give you step-by-step instructions. Continue compressions and follow AED prompts until emergency help arrives or the child starts breathing.
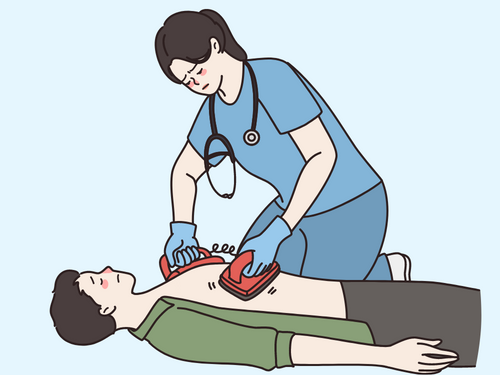
Other emergencies for children and how to respond:
There are other situations in which the child will need immediate help, but CPR is not indicated. In this part of the article, we will discuss the most common emergencies and how to deal with them.
Burns:
Infants and toddlers are more susceptible to deeper burns because their epidermis and dermis are thinner than adults’. On the other hand, because children have less experience and are less able to control their actions, they are more susceptible to burns. Burns cause intense pain and irreversible tissue destruction. Proper initial management can reduce the risk of long-term scarring, which is especially crucial for young children.
Emergency Response:
- Cool the Burn: Immediately place the affected area under cold running water for at least 20 minutes. This eases pain, minimizes swelling, and aids wound healing.
- Remove clothing: Gently remove any clothing covering the burn.
- Seek Medical Help: For severe burns or those involving sensitive areas (face, hands, genitals), call 911.
- Avoid Ice or Rubbing: Do not apply ice (worsens injury) or rub the burn (increases infection risk).
- Cover with a Clean Cloth: Once cooled, cover the burn with a clean cloth or sterile dressing.
Choking:
Choking incidents in infants and toddlers are critical emergencies that demand immediate attention. Infants and toddlers are particularly vulnerable due to their exploratory behavior and tendency to put objects in their mouths. When a child chokes, their airway becomes partly or completely blocked, hindering proper breathing. Lack of oxygen can lead to brain damage or even death if not promptly addressed.
Emergency Response: First, assess the situation. Ask the child, “Are you choking?” If they can breathe, speak, or cough, they might clear the obstruction themselves. If they cannot breathe, cough, or make any noise, act immediately.
- For infants (under 1 year old):
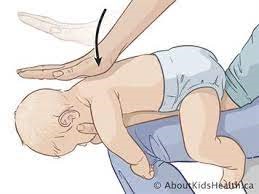
- Back blows: Place the baby face-down on your forearm, supporting their head. Deliver five sharp back blows between their shoulder blades. Check the mouth and remove any visible obstruction.
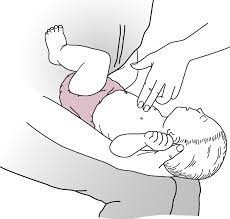
- Abdominal Thrusts (Modified Heimlich Maneuver): Stand in front of the baby. Place two fingers just below the nipple line. Give five quick upward thrusts. Recheck the mouth.
- For Children (1 to 8 Years Old):
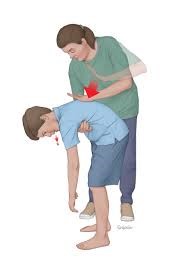
- Back Blows: Support the child’s upper body with one of your hands. Deliver five sharp back blows between their shoulder blades. Check the child’s mouth and remove any visible obstruction.
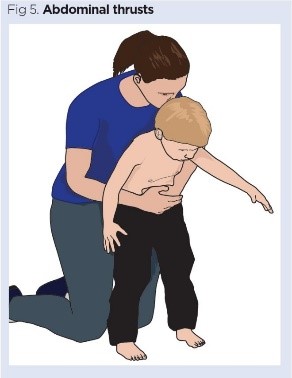
- Abdominal thrusts (Heimlich maneuver): Stand behind the child. Place one hand between the belly button and chest. Use the other hand to deliver five upward thrusts. Recheck the mouth.
Call 911 if the blockage persists. Continue back blows and abdominal thrusts until professional help arrives. If the child becomes unresponsive, assess and start CPR if needed.
Seizures:
Seizures in infants and toddlers are critical events that demand immediate attention. Seizures disrupt normal brain function and can be life-threatening. Lack of oxygen during a seizure can lead to brain damage or even death. A good intervention can prevent complications and improve outcomes.
Emergency Response: Stay Calm. Ensure the child’s safety by moving away any objects that could harm them. Place the child on their side to prevent choking on saliva or vomit. Keep the airway open. Call 911 as soon as you become sure about the child’s safety. During the seizure, avoid restraining the child, and do not put anything in the child’s mouth. Time the seizure. After the seizure is done, keep checking for responsiveness. The child is usually sleepy and tires after a seizure. This is normal and is called a postictal state.
Anaphylaxis:
Anaphylaxis is the most severe form of an allergic reaction. It can rapidly progress and affect a child’s breathing and circulation, leading to shock and even death. Anaphylaxis can be triggered by various allergens, including food proteins (such as egg, peanut, tree nuts, cow’s milk, soy, wheat, fish, shellfish, and sesame), insect bites, medications, and latex (rubber). Approximately one in every 100 school-age children experiences anaphylaxis.
Emergency Response: Recognize the signs. Signs of anaphylaxis include difficulty breathing, wheezing, swelling of the tongue or throat, dizziness, collapse, and pale skin (especially in infants).If you witness these signs, call 911 immediately. Use an adrenaline autoinjector if available. Position the Child, Keep the child lying down with his or her legs elevated; this will help blood circulation in the brain. Loosen tight clothing around the neck. Monitor vital signs. Check your breathing and circulation. Be prepared to perform CPR if necessary.
Head Traumas:
Head injuries can lead to long-term cognitive, behavioral, and physical impairments. Brain development during early childhood makes prompt intervention crucial. Even seemingly minor head trauma can cause brain damage, especially in young children.
Emergency Response: Watch for warning signs. Persistent vomiting, irritability, lethargy, or abnormal neurological findings may be related to a brain injury. Any of these symptoms, especially if they are worsening, requires immediate care. Call 911 and keep checking for the child’s responsiveness.
Authored By:
Dr. Alireza Sarmadi
Family Physician
References:
https://www.redcross.org/take-a-class/cpr/performing-cpr/child-baby-cpr
https://www.redcross.org/take-a-class/cpr/performing-cpr/child-baby-cpr
https://www.cdc.gov/childrenindisasters/helping-children-cope.html
https://info.childcareaware.org/blog/child-care-prepare-infant-toddler-emergency-evacuation
https://www.uptodate.com/contents/moderate-and-severe-thermal-burns-in-children-emergency-management
https://www.sja.org.uk/get-advice/first-aid-advice/choking/child-choking/
https://www.rch.org.au/kidsinfo/fact_sheets/Allergic_and_anaphylactic_reactions/
https://www.healthychildren.org/English/health-issues/injuries-emergencies/Pages/Anaphylaxis.aspx
As a parent or caregiver, our primary responsibility is to make sure our little ones are safe. Accidents may happen at any time, especially to children who are more curious and playful. In this guide, we will discuss essential first aid techniques specifically tailored for infants and toddlers, and young age groups. Fast and informed action can make all the difference when it comes to emergency situations.
In this article, first we will discuss the principles of CPR (Basic Life Support), Then we will discuss other common emergencies in which a child may need immediate help.
Cardiopulmonary Resuscitation:
Infants and toddlers are prone to accidents due to their curiosity and not yet developed motor skills. Common emergencies include falls, choking, burns, allergic reactions, and seizures. As a caregiver, you should be vigilant and look for signs of an emergency.
1. Assess the situation:
The first thing to do when assessing the situation is to make sure that it is safe for you to help the child in need. Assess the environment for hazards such as traffic, sharp objects, or electrical dangers. If all is clear, attend to the child. Check for responsiveness. Gently tap the child’s face and shout to get the child’s attention, use their name if known. Look quickly to see if the child has any injuries, bleeding, or medical problems, do not spend more than 10 seconds at this stage.
If there is no response, check for breathing. Place your ear near the child’s mouth and nose. Your face should be towards the child’s chest. Is there breath on your cheek? Is the child’s chest moving? CPR is indicated only for unresponsive and non-breathing children.

2. Call for help:
As mentioned earlier, if the unconscious child is breathing normally, there is no need for CPR (Cardiopulmonary Resuscitation). Immediately call 911 and ask for help.
If the child is not breathing or is gasping for fresh air, you should start CPR right away.
If you’re not alone, ask the other person to call 911 and then look for an AED as you start the CPR, but if you’re alone, don’t postpone the CPR for calling 911. Start the CPR immediately, and after 2 minutes of effective CPR, call 911 and look for an AED.
3. Start the CPR:
To start the CPR, put the child on a firm, flat surface.
For children under 1 year old, start by placing both of your thumbs in the center of the baby’s chest, just below the nipple line. Use your other fingers to encircle the baby’s chest and provide support. Push down hard and fast. You can also use your index and middle fingers and do the chest compression with one hand, as shown below. The depth of a push should be about one and a half inches. The rate should be 100–120 pushes per minute. Use rescue breaths on a regular basis. If you are alone, the ratio of chest compressions to rescue breaths should be 30:2. If there is another person helping you, the recommended ratio is 15:2.

For performing a rescue breath, tilt the child’s head slightly backwards and lift the child’s chin slightly upwards to make sure the airway is open. Then take a breath, put your mouth around the baby’s mouth and nose to make a seal, and blow gently and steadily for up to one second. The chest should rise. Remove your mouth and watch the chest fall. That’s one rescue breath. You should take two rescue breaths in each cycle.

For Children above 1 year age Place the heel of one hand in the center of the child’s chest, and use your other hand on top, fingers interlaced, and off the child’s chest. Position your shoulders directly over your hands and lock your elbows. Push down hard and fast for about 2 inches at a rate of 100 to 120 compressions per minute. Allow the chest to return to its normal position after each compression. Use rescue breaths with the ratio provided earlier (30:2 if you are alone and 15:2 if there are 2 rescuers).

Check for breath every 2 minutes (every five 30:2 cycles). As mentioned before, if you are alone, you can call 911 and look for AED after about 2 minutes (five cycles).
4: Use the AED as soon as it is available:
For children age 9 and under, use a pediatric automated external defibrillator (AED), if available. If a pediatric AED is not available, or for children age 1 and older, use a standard AED.
First, turn on the AED. Then, wipe the chest dry and attach the pads. The AED will give you step-by-step instructions. Continue compressions and follow AED prompts until emergency help arrives or the child starts breathing.

Other emergencies for children and how to respond:
There are other situations in which the child will need immediate help, but CPR is not indicated. In this part of the article, we will discuss the most common emergencies and how to deal with them.
Burns:
Infants and toddlers are more susceptible to deeper burns because their epidermis and dermis are thinner than adults’. On the other hand, because children have less experience and are less able to control their actions, they are more susceptible to burns. Burns cause intense pain and irreversible tissue destruction. Proper initial management can reduce the risk of long-term scarring, which is especially crucial for young children.
Emergency Response:
- Cool the Burn: Immediately place the affected area under cold running water for at least 20 minutes. This eases pain, minimizes swelling, and aids wound healing.
- Remove clothing: Gently remove any clothing covering the burn.
- Seek Medical Help: For severe burns or those involving sensitive areas (face, hands, genitals), call 911.
- Avoid Ice or Rubbing: Do not apply ice (worsens injury) or rub the burn (increases infection risk).
- Cover with a Clean Cloth: Once cooled, cover the burn with a clean cloth or sterile dressing.
Choking:
Choking incidents in infants and toddlers are critical emergencies that demand immediate attention. Infants and toddlers are particularly vulnerable due to their exploratory behavior and tendency to put objects in their mouths. When a child chokes, their airway becomes partly or completely blocked, hindering proper breathing. Lack of oxygen can lead to brain damage or even death if not promptly addressed.
Emergency Response: First, assess the situation. Ask the child, “Are you choking?” If they can breathe, speak, or cough, they might clear the obstruction themselves. If they cannot breathe, cough, or make any noise, act immediately.
- For infants (under 1 year old):
- Back blows: Place the baby face-down on your forearm, supporting their head. Deliver five sharp back blows between their shoulder blades. Check the mouth and remove any visible obstruction.
- Abdominal Thrusts (Modified Heimlich Maneuver): Stand in front of the baby. Place two fingers just below the nipple line. Give five quick upward thrusts. Recheck the mouth.


- For Children (1 to 8 Years Old):
- Back Blows: Support the child’s upper body with one of your hands. Deliver five sharp back blows between their shoulder blades. Check the child’s mouth and remove any visible obstruction.
- Abdominal thrusts (Heimlich maneuver): Stand behind the child. Place one hand between the belly button and chest. Use the other hand to deliver five upward thrusts. Recheck the mouth.


Call 911 if the blockage persists. Continue back blows and abdominal thrusts until professional help arrives. If the child becomes unresponsive, assess and start CPR if needed.
Seizures:
Seizures in infants and toddlers are critical events that demand immediate attention. Seizures disrupt normal brain function and can be life-threatening. Lack of oxygen during a seizure can lead to brain damage or even death. A good intervention can prevent complications and improve outcomes.
Emergency Response: Stay Calm. Ensure the child’s safety by moving away any objects that could harm them. Place the child on their side to prevent choking on saliva or vomit. Keep the airway open. Call 911 as soon as you become sure about the child’s safety. During the seizure, avoid restraining the child, and do not put anything in the child’s mouth. Time the seizure. After the seizure is done, keep checking for responsiveness. The child is usually sleepy and tires after a seizure. This is normal and is called a postictal state.
Anaphylaxis:
Anaphylaxis is the most severe form of an allergic reaction. It can rapidly progress and affect a child’s breathing and circulation, leading to shock and even death. Anaphylaxis can be triggered by various allergens, including food proteins (such as egg, peanut, tree nuts, cow’s milk, soy, wheat, fish, shellfish, and sesame), insect bites, medications, and latex (rubber). Approximately one in every 100 school-age children experiences anaphylaxis.
Emergency Response: Recognize the signs. Signs of anaphylaxis include difficulty breathing, wheezing, swelling of the tongue or throat, dizziness, collapse, and pale skin (especially in infants).If you witness these signs, call 911 immediately. Use an adrenaline autoinjector if available. Position the Child, Keep the child lying down with his or her legs elevated; this will help blood circulation in the brain. Loosen tight clothing around the neck. Monitor vital signs. Check your breathing and circulation. Be prepared to perform CPR if necessary.
Head Traumas:
Head injuries can lead to long-term cognitive, behavioral, and physical impairments. Brain development during early childhood makes prompt intervention crucial. Even seemingly minor head trauma can cause brain damage, especially in young children.
Emergency Response: Watch for warning signs. Persistent vomiting, irritability, lethargy, or abnormal neurological findings may be related to a brain injury. Any of these symptoms, especially if they are worsening, requires immediate care. Call 911 and keep checking for the child’s responsiveness.
Authored By:
Dr. Alireza Sarmadi
Family Physician
References:
https://www.redcross.org/take-a-class/cpr/performing-cpr/child-baby-cpr
https://www.redcross.org/take-a-class/cpr/performing-cpr/child-baby-cpr
https://www.cdc.gov/childrenindisasters/helping-children-cope.html
https://info.childcareaware.org/blog/child-care-prepare-infant-toddler-emergency-evacuation
https://www.uptodate.com/contents/moderate-and-severe-thermal-burns-in-children-emergency-management
https://www.sja.org.uk/get-advice/first-aid-advice/choking/child-choking/
https://www.rch.org.au/kidsinfo/fact_sheets/Allergic_and_anaphylactic_reactions/
https://www.healthychildren.org/English/health-issues/injuries-emergencies/Pages/Anaphylaxis.aspx
Most Talked About Posts
You May Also Like
Staff Picks
Now Trending
Our Newsletter
Duplicate Email Found!
Well this is embarrassing... It looks like is already registered.
We have just sent an email to that address with a link to manage the subscription with us. If you don't see a message in the next five minutes, check the spam or junk folders, it's definitely there.
See you soon!
Join Our Newsletter
Hey, Thanks For Subscribing!
Please check for a confirmation message and ensure you add us to a safe email list.
If you don't see a message in the next five minutes, check your spam or junk folders and mark our emails safe for next time.
See you soon!
Duplicate Email Found!
Well this is embarrassing... It looks like is already registered.
We have just sent an email to that address with a link to manage the subscription with us. If you don't see a message in the next five minutes, check the spam or junk folders, it's definitely there.
See you soon!










